Topic of the week
WHEN TO SEE YOUR DOCTOR FOR COLD, COUGH AND FLU SYMPTOMS
90% of colds, flu and sore throat are caused by viral infections and usually DO NOT need to be seen by a doctor.
Symptoms of these viral infections might include cough, sneezing, runny or stuffy nose, sore throat, headache, body aches, non-bloody diarrhea, fatigue, and often a low grade fever (below 38◦C or 101◦F). There is no medication that can speed your recovery from a viral upper respiratory infection. Your own immune system will usually fight off the infection in 1-2 weeks, sometimes longer.
Antibiotics can be used for bacterial infections, but will NOT help with viral infections, and maybe harmful. Using NO antibiotics is therefore safer and your infection will get better just as quickly.
Some ideas for helping you feel better during your viral infection:
- rest as much as possible and drink lots of fluid, preferably warm, like tea,
- try ice chips, lozenges, or gargle with salt to reduce throat pain (1 tsp salt in 1 cup of warm water),
- take honey for cough, especially for night time cough in children,
- use cool mist humidifier or vaporizer to add moisture to the air to loosen nasal secretions, and use normal saline nasal spray or gel for stuffy nose,
- Acetaminophen (e.g., Tylenol) or Ibuprofen (e.g., Motrin, Advil) can reduce fever, aches, and pain
- ask your pharmacist for over-the-counter remedies for cough and cold symptoms,
- get a flu shot once you feel better.
See your doctor:
-if you have more than mild symptoms, AND have a chronic medical condition such as asthma, COPD, emphysema, heart disease, diabetes, cancer, inflammatory arthritis or immune disorder
-if you are having shortness of breath or wheezing, or chest pain with breathing
-if you develop a new or higher fever (over 38 C/1001 F), especially with severe headache or neck pain
-if you have thick phlegm that is green or dark yellow, or cough up blood
-if your symptoms are getting worse instead of better
VIRAL INFECTIONS ARE MOST OFTEN SPREAD BY HAND CONTACT, SO FREQUENT HAND WASHING CAN PREVENT THEIR SPREAD.
Workout Injuries: Prevention and Treatment *
A workout injury can happen to anyone, no matter your experience or fitness level. Even walking can cause an injury. But you can significantly cut your risk of getting hurt by following certain workout precautions.
Common Workout Injuries
People hurt themselves in all kinds of ways when they work out. Common workout injuries include:
- muscle pull and strain
- sprained ankle
- shoulder injury
- knee injuries
- shin splint
- tendinitis
- wrist sprain or dislocation
Preventing Workout Injuries
There are simple steps that can help keep you injury-free during your workout. First, if you're a woman over the age of 55 or man over age 45, be sure to check with your health care provider before you start an exercise program. Then you'll be sure you're healthy enough for working out.
Here are guidelines for avoiding injuries during your workout:
Warm-up and cool-down. Every workout should begin with a warm-up and end with a cool-down period. A warm-up helps your body get ready for exercise. It gradually increases your heart rate and loosens your muscles and joints.
Some ways to warm up:
- ride an exercise bike
- jump rope
- jog in place for five to 10 minutes
A cool-down after you work out is important to slowly bring your heart rate back to normal. Walking for five to 10 minutes after you work out is one way to cool down.
Stretch. Stretch before and after you workout. This will:
- increase flexibility
- reduce risk of muscle soreness and injury
It's best to stretch after you warm up and cool down.
Ease into it. When you begin an exercise routine or start a new workout program, start slowly. Then gradually build on the intensity, duration, and frequency.
Don't push yourself too hard. As your fitness abilities increase, you will be able to challenge yourself more.
Cross-train. Vary your workout. Don't overuse one set of muscles. When you repeat the same muscle movements frequently, it can lead to overuse and repetitive-use injuries such as shin splints and tendinitis.
Some ways to vary your workout:
- run on day one
- lift weights on day two
- swim or cycle on day three
Know your trouble spots. Tailor your workout for problem areas. For example, if you have arthritis in your knees, you'll want to build up strength. But don't do exercises that actually hurt. And be sure to start out lightly.
Listen to your body. The "no pain, no gain" philosophy can set you up for an injury. You can get fit without feeling pain. Don't push yourself to the point of pain. If you feel pain, you may be injured. Stop your workout and rest for a day.
Fuel your body. Drink plenty of water before, during, and after you work out. A good rule of thumb is to drink this amount of water:
- 8 ounces about 20 to 30 minutes before working out.
- 8 ounces every 10 to 20 minutes during your workout.
- 16 ounces when your workout is done.
Eat a small meal or snack every two to three hours to keep a steady source of fuel for your body. After your workout, eat a healthy carb and protein snack to replenish your energy stores.
See a trainer. Before starting a weight-lifting or exercise routine, meet with a trainer. He or she can show you how to work out correctly. The trainer will help you create a safe and realistic exercise program.
Dress right. Wear the proper gear for your workout. If you are a runner, wear a good pair of running shoes that fit properly. If you are a biker, always wear a helmet.
Rest: Take one to two days off a week to rest. Rest days give your body a chance to recover between workouts. That can help prevent injuries.
Treating Workout Injuries
Injuries can happen, no matter how careful you are. If you develop a workout injury, follow the RICE method to keep your injury from getting worse:
- R: rest the injury
- I: ice the injury to lessen swelling, bleeding, and inflammation
- C: apply a compression bandage to minimize swelling
- E: elevate the injury to reduce swelling
Nonsteroidal anti-inflammatory medications such as ibuprofen can be taken to ease pain and inflammation from the injury.
Most workout injuries will heal on their own in four weeks or less. If the injury has not improved within a week, or if it gets worse, seek medical care. And always use common sense. If you're concerned about the injury, it's best to seek medical advice.
Until you are fully healed, avoid doing the activity that triggered the injury. And avoid any activity that puts strain on the injured area.
You can still be active as long as you don't stress the injury. Staying active may help you heal quicker than if you take to the couch. Try a new workout while your injury heals. For example, if you sprain your ankle, exercise your arms instead. If you hurt your shoulder, work out your legs by walking.
After you have fully recovered from your injury -- pain-free for more than a week -- start back slowly. Don't try to work out with the same fervor you did before your injury. You will need to rebuild your muscle strength and endurance. It may take three weeks of regular exercise to regain your pre-injury fitness level. If you push too hard and too fast, you may injure yourself again.
----
* Information from WebMD
Viral Gastroenteritis
What is viral gastroenteritis? *
Gastroenteritis means inflammation of the stomach and small and large intestines. Viral gastroenteritis is an infection caused by a variety of viruses that results in vomiting or diarrhea. It is often called the "stomach flu," although it is not caused by the influenza viruses.
What causes viral gastroenteritis?
Many different viruses can cause gastroenteritis, including rotaviruses; noroviruses;
adenoviruses and others. Viral gastroenteritis is not caused by bacteria, or parasites, or by medications, or
other medical conditions, although the symptoms may be similar.
What are the symptoms of viral gastroenteritis?
The main symptoms of viral gastroenteritis are watery diarrhea and vomiting. The affected person may also have headache, fever, and abdominal cramps ("stomach ache"). In general, the symptoms begin 1 to 2 days following infection with a virus that causes gastroenteritis and may last for 1 to 10 days, depending on which virus causes the illness.
Is viral gastroenteritis a serious illness?
For most people, it is not. People who get viral gastroenteritis almost always recover completely without any long-term problems. Gastroenteritis is a serious illness, however, for persons who are unable to drink enough fluids to replace what they lose through vomiting or diarrhea. Infants, young children, and persons who are unable to care for themselves, such as the disabled or elderly, are at risk for dehydration from loss of fluids. Immune compromised persons are at risk for dehydration because they may get a more serious illness, with greater vomiting or diarrhea. They may need to be hospitalized for treatment to correct or prevent dehydration.
Is the illness contagious? How are these viruses spread?
Yes, viral gastroenteritis is very contagious. The viruses that cause gastroenteritis are spread through close contact with infected persons. Individuals may also become infected by eating or drinking contaminated foods or beverages.
How does food get contaminated by gastroenteritis viruses?
Food may be contaminated by food preparers or handlers who have viral gastroenteritis, especially if they do not wash their hands regularly after using the bathroom. Shellfish may be contaminated by sewage, and persons who eat raw or undercooked shellfish harvested from contaminated waters may get diarrhea. Drinking water can also be contaminated by sewage and be a source of spread of these viruses.
Where and when does viral gastroenteritis occur?
Viral gastroenteritis affects people in all parts of the world. Each virus has its own seasonal activity. For example, in the United States and Canada, rotavirus and astrovirus infections occur during the cooler months of the year (October to April), whereas adenovirus infections occur throughout the year. Norovirus infections occur year round but tend to increase in cooler months. Norovirus outbreaks can occur in institutional settings, such as schools, child care facilities, and nursing homes, and can occur in other group settings, such as banquet halls, cruise ships, dormitories, and campgrounds.
Who gets viral gastroenteritis?
Anyone can get it. Viral gastroenteritis occurs in people of all ages and backgrounds. However, some viruses tend to cause diarrheal disease primarily among people in specific age groups. Rotavirus infections are the most common cause of diarrhea in infants and young children under 5 years old. Adenoviruses and astroviruses cause diarrhea mostly in young children, but older children and adults can also be affected. Noroviruses infect persons of all ages, including older children and adults.
How is viral gastroenteritis diagnosed?
Generally, viral gastroenteritis is diagnosed by a physician on the basis of the symptoms and medical examination of
the patient. Rotavirus infection can be diagnosed by laboratory testing of a stool specimen.
How is viral gastroenteritis treated?
The most important of treating viral gastroenteritis in children and adults is to prevent severe loss of fluids (dehydration). This treatment should begin at home by using solutions such as Pedialyte, Equalyte, or sports drinks like Powerade or Gatorade. Medications, including antibiotics (which have no effect on viruses) and other treatments, should be avoided unless specifically recommended by a physician.
Can viral gastroenteritis be prevented?
Persons can reduce their chance of getting infected by frequent handwashing, prompt disinfection of contaminated surfaces with household chlorine bleach-based cleaners, and prompt washing of soiled articles of clothing. If food or water is thought to be contaminated, it should be avoided. Rotavirus gastroenteritis can also be prevented by vaccines.
Is there a vaccine for viral gastroenteritis?
Currently there are two licensed rotavirus vaccines available that protect against severe diarrhea from rotavirus infection in infants and young children. These vaccines are given to children in their first year of life with other childhood vaccines.
* Information from CDC web site http://www.cdc.gov/ncidod/dvrd/revb/gastro/faq.htm
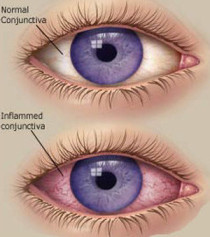
Pink Eye (Conjunctivitis)
Pink, itchy eyes? Pink eye – or conjunctivitis – is common and can spread easily. It sometimes needs medical treatment, depending on the cause. Know the symptoms, when to seek treatment, and how to help prevent it *
Pink eye is one of the most common and treatable eye conditions in children and adults. It is an inflammation of the conjunctiva, the thin, clear tissue that lines the inside of the eyelid and the white part of the eyeball. This inflammation makes blood vessels more visible and gives the eye a pink or reddish color.
What Are the Symptoms of Pink Eye?
The signs and symptoms of pink eye may vary depending on the cause, but they usually include:
- Redness or swelling of the white of the eye or inside the eyelids
- Increased amount of tears
- White, yellow or green eye discharge
- Itchy eyes
- Burning eyes
- Increased sensitivity to light
- Gritty feeling in the eye
- Crusting of the eyelids or lashes
What Causes Pink Eye?
There are four main causes of pink eye:
- Viruses
- Bacteria
- Allergens (like pet dander or dust mites)
- Irritants (like smog or swimming pool chlorine) that infect or irritate the eye and eyelid lining
How Is Pink Eye Treated?
The treatment for pink eye depends on the cause. Pink eye is usually mild and will often get better on its own, even without treatment. However, there are times when it is important to see a doctor and get medical treatment.
Viral Conjunctivitis
Most cases of viral conjunctivitis are mild. The infection will usually clear up in 7–14 days without treatment and without any long-term consequences. In some cases, viral conjunctivitis can take 2-3 weeks or more to clear up, especially if complications arise.
Artificial tears and cold packs may be used to relieve the dryness and inflammation (swelling) caused by conjunctivitis. Antiviral medication can be prescribed by a physician to treat more serious forms of conjunctivitis, such as those caused by herpes simplex virus or varicella-zoster virus. Antibiotics will not improve viral conjunctivitis - these drugs are not effective against viruses.
Bacterial Conjunctivitis
Antibiotics can help shorten the illness and reduce the spread of infection to others. Many topical antibiotics (drugs given as eye drops or ointment) are effective for treating bacterial conjunctivitis. Your doctor may prescribe antibiotic eye drops or ointment as conjunctivitis treatment, and the infection should clear within several days. Artificial tears and cold compresses may be used to relieve some of the dryness and inflammation. However, mild bacterial conjunctivitis may get better without antibiotic treatment and without any severe complications. The use of antibiotics is associated with increased antibiotic resistance and increased costs, and should be a shared decision between the doctor and the patient.
Allergic Conjunctivitis
Conjunctivitis caused by an allergy usually improves when the allergen (such as pollen or animal dander) is removed. Allergy medications and certain eye drops (topical antihistamine and vasoconstrictors), including some prescription eye drops, can also provide relief from allergic conjunctivitis. For conjunctivitis caused by contact lenses, an eye doctor may recommend removing lenses and keeping them out for a period of time. In some cases, a combination of drugs may be needed to improve symptoms.
When to Seek Medical Care
A healthcare provider should be seen if:
- Conjunctivitis is accompanied by moderate to severe pain in the eye(s).
- Conjunctivitis is accompanied by vision problems, such as sensitivity to light or blurred vision, that does not improve when any discharge that is present is wiped from the eye(s).
- Conjunctivitis is accompanied by intense redness in the eye(s).
- Conjunctivitis symptoms become worse or persist when a patient is suspected of having a severe form of viral conjunctivitis—for example, a type caused by herpes simplex virus or varicella-zoster virus (the cause of chickenpox and shingles).
- Conjunctivitis occurs in a patient who has a weakened immune system from HIV infection, cancer treatment, rheumatoid arthritis treatment, or other medical conditions or treatments.
- Bacterial conjunctivitis is being treated with antibiotics and does not begin to improve after 24 hours of treatment.
How Do I Stop Pink Eye from Spreading?
Viral and bacterial pink eye are very contagious and can spread easily and quickly from person to person. By following some simple self-care steps below you can reduce the risk of getting or spreading pink eye. Pink eye that is caused by allergens or irritants is not contagious, but it is possible to develop a secondary infection by other viruses or bacteria.
- Wash your hands often with soap and warm water. If soap and water are not available, use an alcohol-based hand sanitizer that contains at least 60% alcohol.
- Avoid touching or rubbing your eyes.
- Wash any discharge from around the eyes several times a day. Hands should be washed first and then a clean washcloth or fresh cotton ball or tissue can be used to cleanse the eye area. Throw away cotton balls or tissues after use; if a washcloth is used, it should be washed with hot water and detergent. Wash your hands with soap and warm water when done.
- Wash hands after applying eye drops or ointment.
- Do not use the same eye drop dispenser/bottle for infected and non-infected eyes
- Wash pillowcases, sheets, washcloths, and towels in hot water and detergent; hands should be washed after handling such items.
- Avoid sharing articles like towels, blankets, and pillowcases.
- Clean eyeglasses, being careful not to contaminate items (like towels) that might be shared by other people.
- Do not share eye makeup, face make-up, make-up brushes, contact lenses and containers, or eyeglasses.
- Do not use swimming pools.
When Should I Call a Doctor?
Most cases of pink eye are mild and get better without treatment. However, some forms are more severe. Severe cases need to be looked at by a health care provider and may require specific treatment and close follow-up. If you have pink eye, you should see your health care provider if you have:
- Moderate to severe pain in your eye
- Blurred vision or increased sensitivity to light
- Intense redness in the eye
- A weakened immune system, for example, from HIV or cancer treatment
- Bacterial pink eye that does not improve after 24 hours of antibiotic use
- Symptoms that get worse or don't improve
- Pre-existing eye conditions that may put you at risk for complications or severe infection
Pink Eye in Newborns
A newborn baby who has symptoms of pink eye should see a health care provider. Pink eye in newborns can be caused by an infection, irritation, or a blocked tear duct.
Neonatal pink eye caused by sexually transmitted infections, like gonorrhea or chlamydia, can be very serious. If you are pregnant and think you may have a sexually transmitted infection, visit your health care provider for testing and treatment. If you don't know whether you have a sexually transmitted infection but have recently given birth and your newborn shows signs of pink eye, visit your child's health care provider right away.
* From CDCweb site: www.cdc.gov/features/conjunctivitis
Obesity and weight loss management
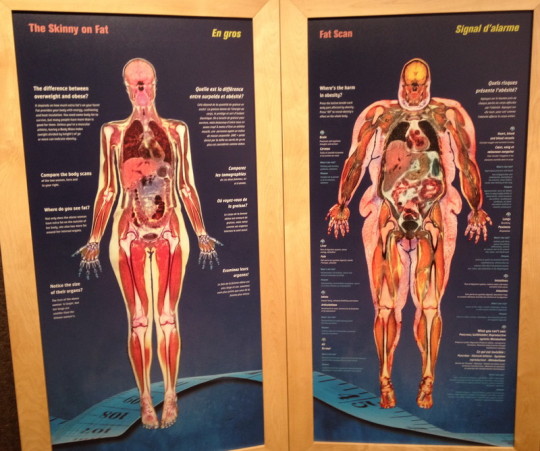
Dangers of Obesity
The image above shows the drastic difference between MRI scans of two bodies - more skinny and more obese. This image is taken at the The AstraZeneca Human Edge exhibition that is now on at the Ontario Science Centre (http://www.ontariosciencecentre.ca/human). This image shows how various organs react and change in overweight body - look at the image and compare how brain, lungs, heart, liver and muscles look on the right and on the left.
Obesity in Canada *
1 in 4 adult Canadians and 1 in 10 children are obese, which means 6 milions Canadians living with obesity require immediate support in managing and controlling their excess weight. Besides bias and discrimination obesity causes type 2 diabetes, high blood pressure, heart disease, stroke, arthritis and cancer. It impacts patient who have obesity, their families, employers, neighbours, health practitioners and governments.
Discrimination based on obesity is comparable to that of racial discrimination, and it’s just as common. Weight bias means inequity in employment, health, health care and education, often due to widespread negative stereotypes that persons with obesity are lazy, unmotivated or lacking in self‐discipline.
One report estimated that direct costs of overweight and obesity represented $6 billion – 4.1 % of Canada's total health care budget. This accounts only for health care costs related to obesity, and does not include productivity loss, reductions in tax revenues or psychosocial costs.
Comprehensive public, private and non-governmental initiatives on obesity prevention and treatment are urgently needed in order to reverse this epidemic.
Read more about obesity and weight loss measures here:
Canadian Obesity Network (http://www.obesitynetwork.ca)
Obesity, Mayo Clinic, US (http://www.mayoclinic.org/diseases-conditions/obesity/basics/definition/CON-20014834)
Obesity in adults, patient UK (http://www.patient.co.uk/doctor/obesity-in-adults)
Weight Loss: Practical Tips **
People become overweight or obese for many reasons. Weight issues can run in families. They can be caused by unhealthy behaviors and a person's environment. Certain health problems and medicines can also lead to unwanted weight gain.
There are some simple things you can do to reach and maintain a healthy weight:
-
Avoid sweet drinks. These include regular soft drinks, fruit juices, fruit drinks, energy drinks, sweetened iced tea, and flavored milk.
-
Avoid fast foods. Fast foods such as french fries, hamburgers, chicken nuggets, and pizza are high in calories and can cause weight gain.
-
Eat a healthy breakfast. People who skip breakfast tend to weigh more.
-
Don't watch more than two hours of television per day.
-
Chew sugar-free gum between meals to cut down on snacking.
-
Avoid grocery shopping when you're hungry.
-
Pack a healthy lunch instead of eating out to control what and how much you eat.
-
Eat a lot of fruits and vegetables. Aim for about 2 cups of fruit and 2 to 3 cups of vegetables daily.
-
Be more active. Small changes in physical activity can easily be added to your daily routine. For example, take the stairs instead of elevators, or park farther away from a store's entrance when you go shopping.
-
Take a walk with your family. A daily walk is a great way to get exercise and to catch up on the day's events.
* from Canadian Obesity Network (http://www.obesitynetwork.ca)
** from American Family Physician (http://www.aafp.org/afp/2010/0615/p1456.html)
Common cold
What is the common cold?
The common cold is one of the most frequent illnesses, leading to more doctor visits and absences from school and work than any other illness every year. Caused by a virus that inflames the membranes in the lining of the nose and throat, colds can be the result of more than 200 different viruses. However, among all of the cold viruses, the rhinoviruses and the coronaviruses cause the majority of colds.
When is the "cold" season?
People are most likely to have colds during fall and winter, starting in late August or early September until March or April. The increased incidence of colds during the cold season may be attributed to the fact that more people are indoors and close to each other. In addition, many cold viruses thrive in low humidity, making the nasal passages drier and more vulnerable to infection.
The rhinoviruses and the coronaviruses are the most common causes of a cold. The rhinoviruses cause about one-third of all colds (30 to 35 percent), while the most common causes of adult colds are the coronaviruses. The same viruses can cause flare of asthma and chronic obstructive pulmonary disease (COPD).
Rhinoviruses - There are more than 110 different rhinoviruses that cause most colds in early fall, spring, and summer. Named after the Greek word "rhin" for "nose," rhinoviruses thrive in the human nasal mucosa.
Coronaviruses - More than 30 different strains of the coronavirus exist, with three or four types affecting humans. The virus is most active in the winter and early spring.
What are the symptoms of the common cold?
The following are the most common symptoms of the common cold. However, each individual may experience symptoms differently. Symptoms may include:
- stuffy, runny nose
- scratchy, tickly throat
- sneezing
- watering eyes
- low-grade fever
- sore throat
- mild hacking cough
- achy muscles and bones
- headache
- mild fatigue
- chills
- watery discharge from nose that thickens and turns yellow or green
Colds usually start two to three days after the virus enters the body and symptoms last from several days to several weeks.
The symptoms of the common cold may resemble other medical conditions. Always consult your physician for a diagnosis.
How is the common cold spread?
The common cold is highly contagious. It is often spread through airborne droplets that are coughed or sneezed into the air by the contagious person and then inhaled by another person. Colds can also be spread by hand-to-hand or hand-to-infected-surface contact, after which a person touches his/her face.
How is a cold different from the flu?
A cold and the flu (influenza) are two different illnesses. A cold is relatively harmless and usually clears up by itself after a period of time, although sometimes it may lead to a secondary infection, such as an ear infection. However, the flu can lead to complications, such as pneumonia and even death. What may seem like a cold, could, in fact, be the flu. Be aware of these differences:
| Cold Symptoms | Flu Symptoms |
|---|---|
| Low or no fever | High fever, above 102F or 39C, lasting 3-4 days |
| Sometimes a headache | Always a headache, often comes suddenly |
| Stuffy, runny nose | Clear nose |
| Sneezing | Sometimes sneezing |
| Mild, hacking cough | Cough, often becoming severe |
| Slight aches and pains | Often severe aches and pains |
| Mild fatigue | Several weeks of fatigue |
| Sore throat | Sometimes a sore throat |
| Normal energy level | Extreme exhaustion |
Who is at greater risk for catching the common cold?
Children suffer more colds each year than adults, due to their immature immune systems and to the close physical contact with other children at school or daycare. In fact, the average child will have between 6 to 10 colds a year, while the average adult will get 2 to 4 colds a year. However, the average number of colds for children and adults will vary.
Prevention for the common cold:
The best way to avoid catching the common cold is to wash your hands frequently and avoid close contact with people who have colds. When around people with colds, do not touch your nose or eyes, because your hands may be contaminated with the virus.
People with colds should cough and sneeze in facial tissue and dispose of the tissue promptly, and then wash his/her hands immediately. In addition, cleaning surfaces with disinfectants that kill viruses can halt the spread of the common cold. Research has shown that rhinoviruses may survive up to three hours outside of the nasal mucosa.
How is the common cold diagnosed?
Most common colds are diagnosed based on reported symptoms. However, cold symptoms may be similar to certain bacterial infections, allergies, and other medical conditions. Always consult your physician for a diagnosis.
Many people believe taking large amounts of vitamin C will either prevent the common cold or reduce its symptoms. However, to date, studies have not indicated that high amounts of vitamin C affect the onset and symptoms of the common cold. In addition, taking large quantities of vitamin C over a long period of time may, in fact, be harmful, causing diarrhea and distorting urine and blood test results.
Treatment for the common cold:
Currently, there is no medication available to cure or shorten the duration of the common cold. However, the following are some treatments that may help to relieve some symptoms of the cold:
- over-the-counter cold medications, such as decongestants and cough medicine
- over-the-counter antihistamines (medication that helps dry up nasal secretions and suppress coughing)
- rest
- increased fluid intake
- pain relievers for headache or fever
- warm, salt water gargling for sore throat
- petroleum jelly for raw, chapped skin around the nose and lips
- warm steam for congestion
Note: Because colds are caused by viruses, treatment with antibiotics is ineffective. Antibiotics are only effective when given to treat bacterial infections.
Do not give aspirin to a child who has fever without first contacting the child's physician. Aspirin, when given as treatment for viral illnesses in children, has been associated with Reye syndrome, a potentially serious or deadly disorder in children. Therefore, pediatricians and other healthcare providers recommend that aspirin (or any medication that contains aspirin) not be used to treat any viral illnesses (such as colds, the flu, and chickenpox) in children.
Complications from colds:
Colds can lead to secondary infections, including bacterial middle ear and sinus infections that may require treatment with antibiotics. When a cold is accompanied by high fever, sinus pain, significantly swollen glands, or a mucus-producing cough, a complication may be present that requires additional treatment.
Cold weather and colds:
Contrary to popular belief, cold weather or getting chilled does not cause a cold. However, more colds do occur during the cold season (early fall to late winter), which is probably due to a variety of factors, including:
- schools are in session, increasing the risk for exposure to the virus
- people stay more indoors and are in closer proximity to each other
- low humidity, causing dry nasal passages which are more susceptible to cold viruses
*Sources: Public Health Agency of Canada, The Ohio State University Wexner Medical Centre web page